A dentist has spoken of the difficulties faced throughout the pandemic, including the rationing of procedures – which led to some patients unnecessarily losing teeth.
Urgent dental care centres (UDCCs) were set up by health boards across Scotland at the start of the first lockdown when dentist practices were closed.
But while patients in pain were treated at these centres, only limited aerosol-generating procedures could be carried out.
Strict rules were brought in to regulate the use of drills, and other tools, which could cause droplets to spray from a patient’s mouth.
Ultimately, the reduced services meant some people were faced with losing teeth which could have been saved had there been no pandemic.
‘Patients ended up losing teeth that might have been otherwise restorable’
Eddie Bateman, who owns Tain Dental Care in Ross-shire, volunteered at a UDCC in the Highlands.
Eddie was one of three health professionals speaking of problems services have faced over the past year at an NHS Highland board meeting this week.
He said: “As things moved on, aerosol-generating procedures became available at UDCCs, but they were rationed.
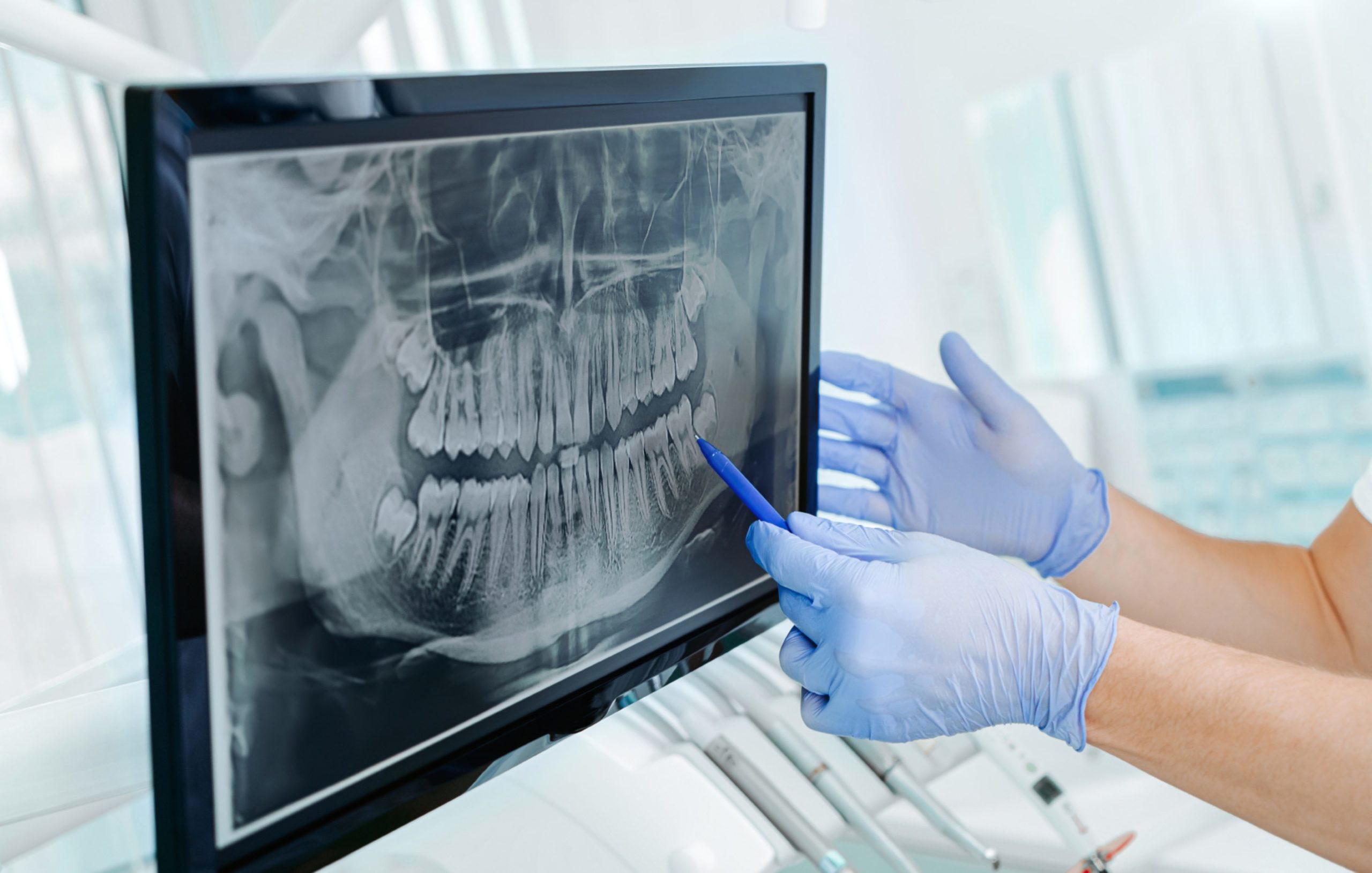
“So because there wasn’t enough capacity we found that lots of our patients ended up losing teeth that might have been otherwise restorable in different situations.”
The meeting also heard from pharmacists who told of pharmacies running out of medicines, PPE being in short supply at the start of the outbreak, and the difficulties health workers tackled as they had to adapt to ever-changing rules and guidelines.
Robots were even drafted in to dispense drugs as the NHS looked to improve their ways of working.
‘One of the most satisfying parts of our job is getting people out of pain, but having that withdrawn from us was difficult’
Eddie said he spent “sleepless nights” figuring out redundancies at his work until the furlough scheme was announced.
“Constant change was another factor,” he explained. “Often these changes were announced by politicians to the public on television before the profession.
“So the first we would hear would be a phone call to the receptionist asking if they could book a check-up, which wasn’t ideal.
“It was difficult because one of the most satisfying parts of our job is getting people out of pain, but having that withdrawn from us was difficult.
“Particularly where working in a rural setting where, unavoidably, a lot of our patients are our friends phoning up looking for help which we couldn’t provide.”
Dental staff have quit because it’s not the job they signed up for
Wearing enhanced PPE for aerosol-generating procedures has also been a challenge for staff with many feeling burnout because of it.
Eddie said: “This year, for example, I’ve had three members of staff who have been with me for seven years, or since I opened the practice, who decided to leave just because it’s not the job that they signed up for and they find it a lot more difficult now.”
The health board heard that dentists across Scotland were still operating at a third of their normal level of patients in May.
Community pharmacies faced drug shortages
Catriona Sinclair, a community pharmacist from Strathpeffer, also spoke at the board meeting and said the first two months of the pandemic were the “biggest challenge”.
She said: “Community pharmacies stayed open from day one of the pandemic and we were overrun with patients who, understandably, panicked at the thought of not being able to get access to medicines.
“Everybody wanted to clear our shelves so we had an extremely hectic few months.
“Some of the items did go short so that took up a lot of the pharmacist’s time. Inhalers is an example because the drug companies weren’t expecting an increase, so the warehouses didn’t have the stock and we couldn’t get the stock.
“The knock-on down the supply chain was phenomenal.”
The roles of community pharmacists have continued to develop throughout the pandemic with many now qualified to issue prescriptions for certain conditions.
Clinical teams were stockpiling end of life drugs
Rhona Gunn, associate director of pharmacy, spoke of the experiences of staff working in the department during the pandemic at Raigmore Hospital.
“We knew when it started – because there was information coming from the Italian experience – that we were likely to have significant issues with medicine supplies.
“Everyone was trying to get the same medicines at the same time.”

She said clinical teams were stockpiling important drugs such as end-of-life care medicines in case they ran out.
Two robots were also drafted in to work in the pharmacy department at the hospital to dispense medicines, which gave staff more time to work with patients.
The machines are capable of accurately dispensing and managing large quantities of medicine supplies.
Technology will be key moving forward
However, the biggest challenge the department faced and still faces is the recruitment and retention of staff.
“At the moment between annual leave, vacancies, sick leave and self-isolation we’re running at about 55% of our establishment which has been incredibly tiring for staff,” she said.
“Moving forward the big thing is to continue the transformation of our services to try to be able to improve those services for patients, and also do it in a more sustainable manner.
“Technology is going to be one of those things that we do around that.”
Other health and wellbeing stories you may like…
NHS Grampian reveals future plans for the health service
NHS boss explains why we should keep wearing face masks
Ex-TOWIE star reveals eptopic pregnancy shock



